Home › magazine › special features › The holy grail
The holy grail
15th of September 2010Mike Sullivan, managing director of GOJO Industries, addresses specific hand hygiene requirements for healthcare workers and outlines how compliance is key to implementing a successful programme.
The role of hand hygiene in helping to prevent the spread of viruses and infections has been universally acknowledged. International organisations and authorities together with manufacturers such as GOJO have been particularly active in issuing guidance in recent years to help reduce the number of healthcare acquired infections.
Providing advice and training on specific hand hygiene requirements for those working in healthcare environments is very much part of our service, helping prevent the spread of infections by hand whilst increasing awareness of the importance of hand hygiene to keep skin healthy.
Some of the most frequent questions asked around implementing a successful programme for healthcare workers include how often and for how long personnel should wash their hands, the types of products recommended in this environment, the importance of hand drying and how to engage and motivate staff to fully adhere to good hand hygiene practice on an ongoing basis.
Hand hygiene compliance is the overriding principal threading through these questions. With everything you do or implement you must ask yourself how it will help staff comply with best practice and help instil a behaviour change that will motivate this single most important act to reduce the spread of infection. Compliance needs to drive every step of the hand hygiene programme and if it is not addressed then this is inevitably where standards will fall.
In our experience problems with compliance relate directly to time restrictions, skin irritability, lack of facilities, sparse education or awareness and motivation.
Consequences of hand washing
Wearing gloves, contact with detergents and other chemicals and bad hand hygiene practice can all contribute to causing damage to the outer layer of the skin - the epidermis. Skin irritation is one of the most common problems faced by healthcare workers today as they strive to constantly keep hands clean and deter workers from sticking to a correct hand hygiene regime.
Continuous hand washing removes the surface oils from the skin, allowing moisture to escape and hands to eventually become dry. Likewise wearing gloves prevents moisture escaping from the skin and damages the oily layer making it more vulnerable to drying out.
Severe cases are classed as ‘irritant contact dermatitis’ and typical symptoms include redness, dryness, blistering or itching. Sometimes it may be mistaken for an allergy but instead occurs as a result of the skin breaking down and cracking because of a reduction in moisture. The skin is then unable to act as a barrier and opens up allowing chemicals and bacteria to penetrate.
Without proper attention and guidance in place, dry skin will eventually turn sore and cracked which makes the worker prone to the spread of infection and in severe cases can potentially lead to absenteeism of the individual from work.
To stop this vicious circle it is important to develop an effective hand hygiene programme for healthcare workers who need to keep their hands clean throughout the day.
Rules of a good skin care regime
It is estimated that 80 per cent of infections are transported by hands, making hand washing the single most important procedure for preventing the spread of pathogens.
For clinical staff the failure to wash hands before and after each patient contact is probably the most important contributor to the spread of infections, whereas cleaning staff should wash their hands to prevent cross contamination between areas.
The challenge here is keeping skin clean and soft to encourage compliance. This can be achieved by washing hands at the right times and in the right way by following a few simple rules.
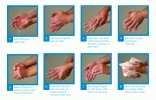
Hands should be washed when they are visibly soiled. Proper hand washing involves vigorous motion with the hands rubbing together and fingers working in between the finger spaces. About 15 to 20 seconds of hand washing is recommended to remove germs.
Always wet hands before applying soap. This dilutes the detergent in the soap and helps to reduce the defatting effects. Take only the recommended dosage from the dispenser and use the mildest soap possible. GOJO can help recommend the correct products for all working environments.
Lukewarm water should be used because hot water reduces the skin’s ability to work as a barrier. Over time this may lead to dryness.
Carefully rinse hands to wash away all of the soap and remove and soap residual that overtime may act as an irritant.
Hand drying is a key factor in developing effective hand hygiene practices yet in a busy healthcare environment it can often be overlooked. The danger of insufficient hand drying is that it can render the hand washing process ineffective.
Evidence supports the use of paper towels as the most efficient method for reduction in contamination. Use the paper towel to blot away water being careful not to scrub the hands as this can remove layers of skin cells leaving it prone to dryness.
To help restore the skin’s natural oils, it is then advised to use a moisturising lotion. Without a suitable emollient or moisturiser for staff to use at break times or at the end of a shift the skin will quickly lose its natural hydration and protection, which actually increases the risk of colonisation by micro-organisms and could cause illness. A water based emollient can penetrate the outer layers of the skin and help maintain conditions which optimise the skin’s own natural functions.
It is important to understand when to wash and when to sanitise. Pathogens react to different methods of removal. For instance, some sporicidal pathogens are effectively removed by friction of hand washing, whilst other more transient germs can be effectively removed by use of an alcohol gel.
It is very easy to fall into a false sense of security by amending the protocols and good practice of hand hygiene to suit the need of the immediate outbreak. A good regime will ensure that hospital protocols are followed in a case of an outbreak, but will not forego consistent awareness and hand hygiene practices that may allow other pathogens to surface and thus become dangerous.
AT GOJO our education programme will highlight the do's and don’ts but recommend washing when hands are visible soiled, using an alcohol rub when soap and water are not available or at point of patient care and keeping hands moisturised.
The role of alcohol gels
Time is of the essence for healthcare workers as they rush from patient to patient or strive to keep wards clean. Hands that are visibly soiled must be properly washed and thoroughly dried but alcohol gels can be used as required to complete the procedure at point of patient care as recommended by the World Health Organisation’s 5 moments of hand hygiene.
Sanitisers such as PURELL, can be used when hands are clean but it is necessary to kill germs on the hands to prevent cross contamination. A high level alcohol gel or rub has to be effective against 99.99 per cent of most common germs that may be harmful.
Alcohol gel dispensers, combined with wash facilities, should be placed in the right locations throughout the healthcare setting to encourage use and deter non-compliance. Hospitals are increasingly placing dispensers in reception areas to show their commitment to hand hygiene and there is an increase in the educational awareness to visitors to encourage them to also sanitise their hands when entering the hospitals and wards.
Healthcare workers may also benefit from wearing a small bottle of gel attached to their waistband using a retractable clip to make it even more convenient to sanitise on the go and demonstrate responsibility to protect themselves and others around them from infection.
Engaging and motivating staff
Healthcare workers need to be engaged because while they may be presented with convincing data for hand washing as an infection control preventative activity, it remains an activity of self-monitoring. Risk assessments and surveillance methods can be put in place but best practice will be achieved by getting healthcare workers to really understand the issues.
GOJO have an established team of experts whose sole focus is on-going support to hospitals across Europe. Combining advice on recommended product regimes, educational materials and site visits, they provide a total and bespoke solution to ensuring the correct hand hygiene protocols are being implemented.
One issue regularly addressed is education. To achieve compliance this needs to involve more than simply putting up a poster. Healthcare workers must be constantly kept up to date on hand decontamination issues. In our experience the message should be fresh and tailored towards different audiences within the healthcare environment. Repetition of the same message in the form of sales materials and visuals being used could lead to the message being ignored.
To conclude then, the effects of hand washing in the prevention of disease transmission from person to person are undeniable but the key to success is to focus on effective compliance. The choice of hand washing rests with the individual in the battle against the transmission of disease or infection. Helping personnel address compliance issues and keeping them up to date with the latest developments in hand hygiene will help maintain and improve best practice in a bid to continue reducing hospital acquired infections.
• PURELL is a trademark of Johnson & Johnson and is used under license.